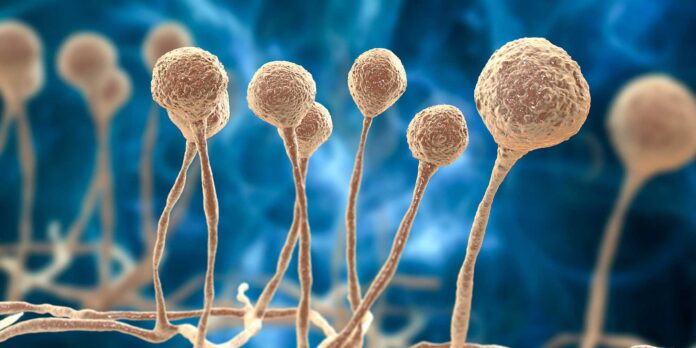
As COVID wreaks havoc on our world, another infection has been slowly creeping up and killing lives. Although the black fungus only appears in a handful of cases for the past years, COVID-19 has made it possible that there are thousands of deaths due to black fungus.
What Is Black Fungus?
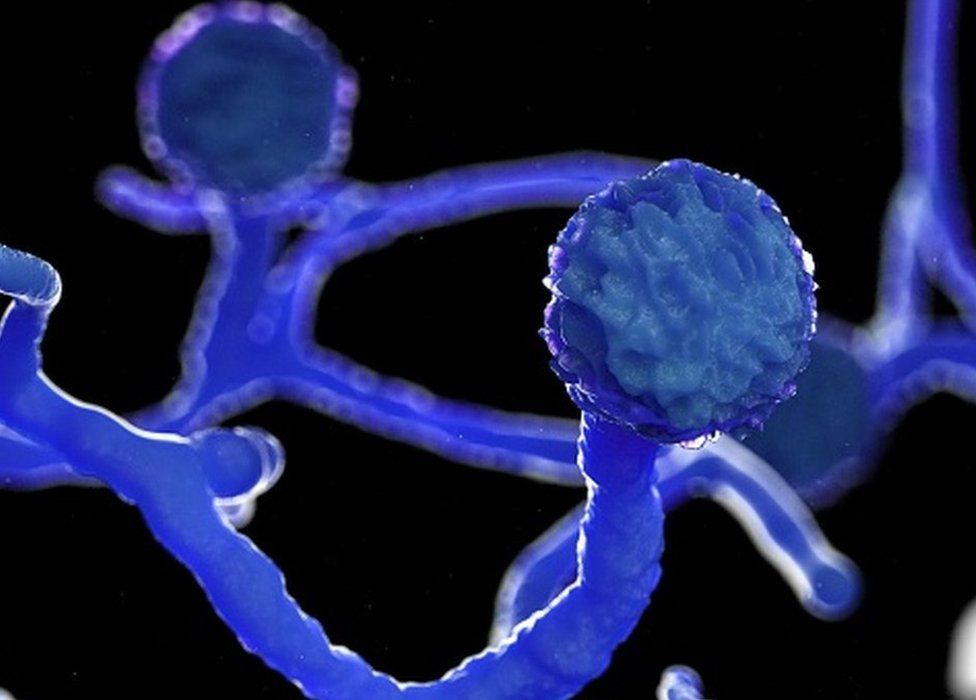
Black fungus or also known as Mucormycosis is a rare fungal infection from prolonged exposure to mucor mould which is something that’s present in the environment. Before the COVID-19 pandemic, the infection isn’t common. But as the pandemic looms in our community, its numbers have gotten higher.
What to know about mucormycosis
Mucormycosis is a rare, invasive, fungal opportunistic infection that would sometimes lead to serious, fatal disease. Those who are most at risk for mucormycosis have compromised immune systems that make them susceptible to fungal and other infections. These symptoms are present on individuals who are currently fighting or have recently recovered from COVID-19 disease.
Over the last 10 years, mucormycosis has only been seen by the handful in India. This past month, however, tens of thousands of cases have been reported. With India’s health resources stretched to a limit due to COVID-19, the black fungus adds to an already full plate on the hands of the government.
What Are The Symptoms Of Black Fungus?
The infection can manifest by way of
- Pain in the eyes
- Severe headache
- Discoloration or blackening of tissue on nose and cheeks
- Congestion in the nose
- Loss or blurred vision
- Toothache
- Swelling in eyes or cheeks, and
- Bleeding from the nose
How does one catch black fungus?
Black fungus can infect people via fungal spore floating in the environment. An easy way for one to be infected is when the fungus enters the skin through a cut, burn, or other types of skin trauma. After coming in touch, the fungus sticks to a body part, then travel inwards through the nose, sinus or lungs.
If the fungus goes in through a cut or burn, then it infects the wound locally. Yet if it goes through the sinus, it can affect the eyes and eventually, the brain, leading to a fatal condition.
There are many ways that the black fungus can infect the body of thousands of people, but there are some theories to how this can happen. Some doctors think that black fungus infected people when medicines were administered to at-home COVID patients that do not have their blood sugar levels under control.
Other share the theory that the black fungus was able to infect people due to immune systems that were suppressed due to drugs, with unclean, unhygienic post-COVID living conditions of patients.
It was thought that doctors who are under pressure and patients in panic are making the situation worse. Physicians who are desperate for the survival of their patients may choose aggressive medical treatments instead of being conservative, which may contribute to the suppressing of immune systems.
Mucormycosis cases are also thought to be arising because of overuse of cheap steroids which are used in order to bring exaggerated inflammatory response to covid under control. Steroid suppress immune response, which can increase vulnerability to secondary infections like black fungus.
Not only that, but another theory mentions the use of ordinary tap water in flow meters of oxygen cylinders is also being blamed for such fungal infections. Cases may be triggered by “mold-tainted oxygen pipes and humidifiers”.
Can Black Fungus Be Treated?
Once a person has been infected by the fungus, it spreads through the nose, attacks the eyes, and eventually reaches the brain. For that reason, precautions must be taken before the infection reaches the brain because once it does, it becomes difficult to treat and decreases the patient’s chances of survival.
Treatments are severe, for the affected tissues must be surgically removed and can leave people disfigured. Patients end up losing their eye/s and even their upper jaw. Precaution and prevention is the key here, which is why it’s important to be attentive. After a consultation with a doctor, those who are infected will be given a combination of steroids. But that is not all as you will need to closely monitoring one’s blood sugar levels. Depending on the level of severity of the fungal infection, a doctor may also recommend an intravenous anti-fungal procedure spanning four to six weeks.
How risky is this condition?
The condition is very dire for the patients, with, mortality is as high as 80% for an untreated patient or remains untreated long. If treated, it is still 40-50% chance. Patients will mostly recover if the infection is caught at the sinus stage. But that doesn’t mean that there will be no side effects to the drugs, as reported side effects can include kidney issues, neurological dysfunction and stroke.